Areflexia
Definition and Clinical Presentation
Areflexia is the complete absence or loss of deep tendon reflexes (muscle stretch reflexes). While hyporeflexia denotes a diminished or sluggish reflex, areflexia indicates that no reflex muscle contraction can be elicited, even with reinforcement techniques. It can be a physiological variant in a small percentage of healthy individuals who naturally lack tendon reflexes, but it is far more commonly a pathological sign indicating dysfunction in the peripheral or central nervous system.
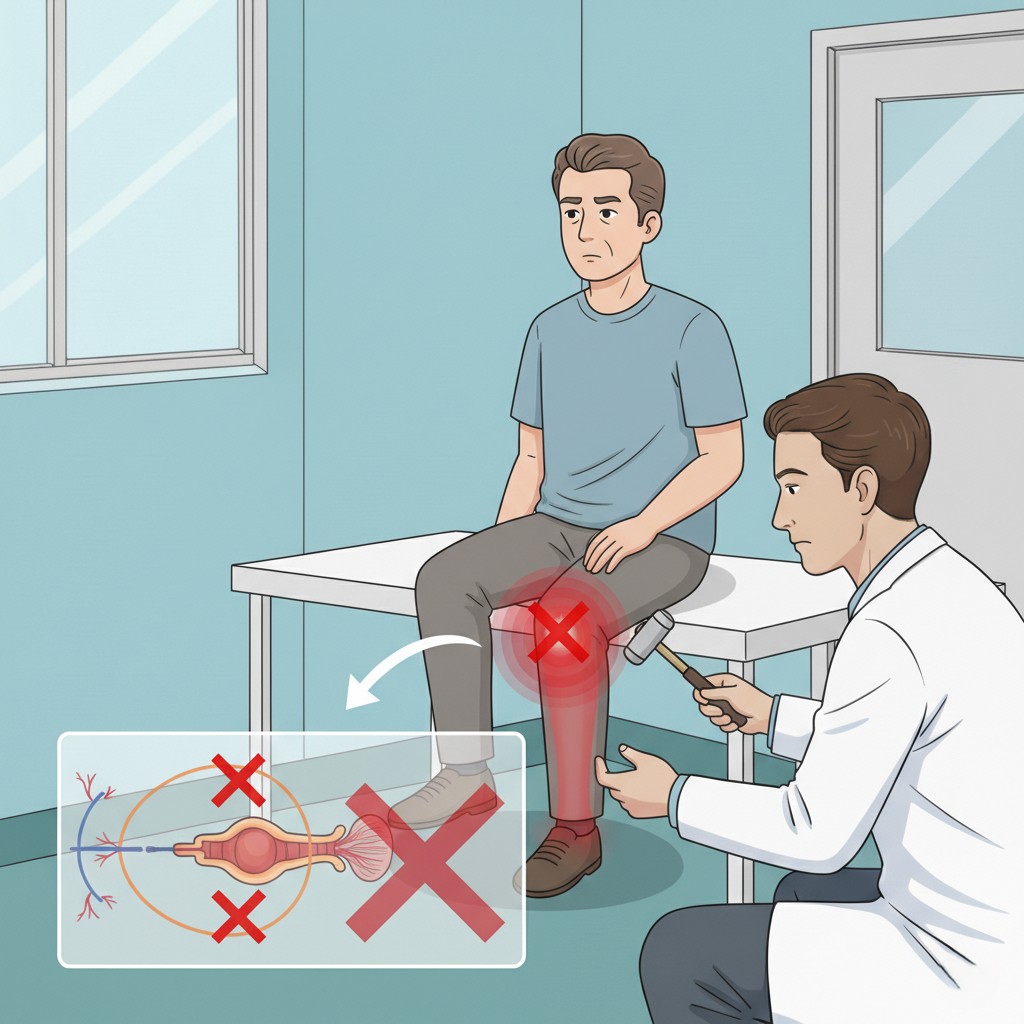
A lesion anywhere along the monosynaptic reflex arc—including the sensory afferent fibers, spinal cord segment, or motor efferent pathways—can result in areflexia.
Pathophysiology and the Reflex Arc
Pathological areflexia reflects an anatomical interruption or physiological dysfunction at any point along the monosynaptic reflex pathway, which serves as the neuroanatomical substrate for phasic stretch reflexes. The normal mechanism is as follows:
- A sudden tendon stretch (produced by a sharp blow from a tendon hammer) activates muscle spindle receptors.
- This signal is transmitted via Ia sensory afferent fibers to the dorsal root ganglion and into the spinal cord.
- In the ventral horn of the spinal cord, the sensory neuron synapses directly with an α-motor neuron.
- The α-motor neuron sends an efferent signal back to the muscle, causing it to contract and completing the monosynaptic arc.
Because the reflex arc requires both sensory and motor components, areflexia is not exclusively a motor sign. It frequently occurs in pure "sensory" neuropathies that selectively damage the large-diameter Ia afferent fibers from the muscle spindle.
Causes and Associated Conditions
Areflexia is primarily a hallmark of lower motor neurone (LMN) syndrome, but it can arise from several distinct pathophysiological categories:
- Peripheral Neuropathies: Both axonal and demyelinating neuropathies commonly cause widespread areflexia. A classic example is Guillain-Barré syndrome (Acute Inflammatory Demyelinating Polyradiculoneuropathy), where areflexia is a required diagnostic criterion.
- Radiculopathies and Plexopathies: Compression or injury to specific nerve roots or nerve plexuses will cause focal areflexia corresponding to the affected segment (e.g., an absent ankle jerk in an S1 radiculopathy).
- Neuromuscular Junction Disorders: In Lambert-Eaton myasthenic syndrome (LEMS), reflexes are characteristically absent at rest. However, they may be transiently "restored" immediately following a brief period of maximum voluntary muscle contraction—a phenomenon known as post-tetanic facilitation.
- Central Nervous System Disorders: While central lesions typically cause hyperreflexia, acute central injuries can produce transient areflexia. This is classically seen in "spinal shock" immediately following acute spinal cord compression or severe traumatic spinal injury. Transient areflexia is also a defining clinical feature during an episode of cataplexy.
Clinical Examination Technique
When assessing for areflexia, the clinician must ensure that the patient is fully relaxed. Before concluding that a reflex is truly absent, reinforcement techniques, such as the Jendrassik maneuver (asking the patient to hook their hands together and pull forcefully while the reflex is tested), must be employed to heighten anterior horn cell excitability.
Experienced clinicians often note that they can "hear" areflexia; when the reflex is completely absent, striking the tendon produces a dull, unyielding "thud" of the hammer against the tendon and bone, devoid of the characteristic visual or palpable muscle twitch.
Cross References
Cataplexy; Facilitation; Hyporeflexia; Lower motor neurone (LMN) syndrome; Plexopathy; Radiculopathy; Reflexes
